Activated patient? The phrase sounds like something which might explode, as if you had a sleeping bomb that suddenly became unpassive, unlimp and willing to take part in its own health.
To some doctors the activated patient program sounds rebellious. It teaches everyday folks everything from taking their own blood pressure to replacing commercial nose drops with a homemade salt solution.
Said one suspicious doctor: “I object to the term. It implies that the patient should get into rebellion against the doctor.”
But Dr. Keith W. Sehnert said he has known only one case of opposition to the program he started which has spread to 3,000 graduated patients in 37 states. A physician in Galveston, Tex., was reprimanded by his medical society for teaching it recently, he said.
Dr. Sehnert’s definition of the activated patient comes from his book How to Be Your Own Doctor (Sometimes). It describes an individual “whose clinical skills and understanding of his health are such that he becomes an active participant in his own health care in contrast to the passive role traditionally assigned him.”
“We’re not as stupid as we have pretended to be,” said Mrs. Reta Morrill, 45, mother of five and resident of Peak’s Island, a 20-minute ferry ride off the coast of Maine. “We’re not such dumb creatures after all.”
Mrs. Morrill was interviewed along with other women graduates of the 20-hour course given by the community medicine department of Maine Medical Center, the state’s largest hospital, in Portland.
Peak’s Island and another island–Chebeague–were picked for activated patient courses because of their rural nature and because they couldn’t support a full-time physician. Chebeague is the second largest of the Casco Bay Islands and has 350 year-round residents and 1,500 in the summer. Many are retired business executives. Peak’s has 1,000 residents year-round and 5,000 in the summer with a full-time nurse practitioner working out of the Casco Bay Health Center. It was there I interviewed the women graduates of the course in a tiny office of the nurse practitioner, Marjorie Erico.
Mrs. Jean Dinsmore, 26, of Peak’s Island, a mother of three, said that one evening during the course a pharmacist urged her to throw out most of a shopping bag full of prescription and non-prescription drugs gathered from her medicine cabinet as part of the assignment. The drugs included valium, stellazine, artarre, sudafed cough syrup, actifed, demitap and other kinds of cough medicines and many kinds of aspirins.

On Chebeague, Mrs. Trudy Burrill, 60, a retired school teacher and one of the 24 students in the course held there last fall, said that the course gave her confidence and a better attitude toward herself. She said a doctor told her that the best thing for a cough was “loads of water, which is better than cough medicine.” She was traveling in Morocco with her husband, caught a cold, and drank plenty of water and wine and got better. Compliments of the activated patient course? Yes, she says.
Ned Morse, president of the Chebeague Island Council which has been seeking a doctor and a clinic for the island, said what he got most from the course was learning how to brush his teeth.
“Instead of going up and down with a big hard brush, I use a soft brush that gets between the gums,” he said adding that “once a day is enough and toothpaste isn’t necessary. Only use it if you like the taste.”
I reached Chebeague by an hour ferry ride from Portland on a gem-like day. Morse met me at the ferry landing and we toured the island, which means Isle of Many Springs in Indian, before a lunch in the new living room addition of a converted farmhouse belonging to Carolyn and William Swann, a retired executive from Eastman Kodak.

Morse had arranged for six graduates of the course to sound off on their feelings about the course and how it helped them. They finished the 20-hour course in December, meeting from 5:30 to 7:30 P.M.
The course was based on Dr. Sehnert’s program. (He is visiting professor of Health Activation Programs at the School of Nursing, Georgetown University, Washington, D.C.). But it was coordinated locally by the department of community medicine of the Maine Medical Center in Portland, represented by Dr. J. Michael Taylor, department head, and Eleanore M. Irish, R.N.


The ten 2-hour sessions covered:
- The concept of the activated patient and partnership with the health care provider, and self care activities from exercise to sleep and food habits.
- “Your Medicine Chest,” one of the most popular evenings, was given by a pharmacist who is spare with drugs. He had each student bring in the medicines they have at home in shopping bags to impress upon them how many they had accumulated. The pharmacist, Robert R. Auger, who is director of pharmacy services at the hospital, said that medicine cabinets should not be kept in bathrooms which are moist and steamy but in high, dry cabinets away from children, away from moisture and away from heat.
Auger also told students to be wary of old iodine which can burn the skin if the alcohol has partly evaporated. Mercurochrome and tincture of Merthiolate he called “psychological paint” and urged them to throw them out.
One Chebeague native, Beth Smith, 26, said her husband objected to chucking the Merthiolate. “I told him it is better to wash out a cut with water and soap and keep it clean, but he felt better with the Merthiolate,” she said.
Husband pressure took hold on Peak’s Island when Dot Flynn, 52, said her husband, John, a retired acting fire chief from Portland, handpicked the medications she took to the class and wouldn’t let her clean out the family medicine cabinet.
Auger himself keeps only Tylenol, mouthwash, bandaids, and vitamin B complex in his own medicine closet. He suggested a saline solution of one teaspoon of salt to a quart of water as a substitute for commercial nose drops which can dry out the mucus membranes if used more than four days. He stressed that there was a place for nose drops but the problem is that people who start using them tend to stay on them too long.
He urged students to avoid double strength aspirin at premium prices and to buy the generic from Squibb and Parke Davis which are cheaper because they don’t advertise it. To see if aspirin has outlived its usefulness unscrew the cap and sniff. If you get a strong vinegar smell it means it is decomposing and losing its strength. He stressed strong smell, because all aspirin has a slight vinegar smell. He said if customers bought smaller sized bottles instead of the large economy size they would run less risk of those going bad. The vinegar smell comes from acetylsalacitic acid.
The class was urged to shop around by phone to different pharmacies before buying a drug. Auger also suggested establishing oneself with one pharmacist who can maintain a patient profile listing one’s allergies. He can keep track in case two physicians prescribe the same drug by two different names causing a possible overdose.
Auger warned against mixing outdated drugs in the same bottle. If you mix penicillin with aspirin and give the aspirin to someone allergic to penicillin the aspirin might have picked up enough to cause a reaction. “People should leave the original drug in the original bottle and not mix them together,” he said.
Each person was asked to list the number of his or her poison control center. Mrs. Dinsmore on Peak’s Island said that when her 2-year-old swallowed 25 Fluoride tablets (she knew the amount in the bottle), she kept calm and called the center. Patient activation stresses that knowledge helps avoid panic and she didn’t. The center assured her not to worry unless there were more than 50 pills.
At the Peak’s Island session on the medicine chest (the course content varies between the islands), Thomas R. Scarponcini, staff pharmacist at the hospital, told of common poisonous plants including tomato and potato leaves and of course the better known rhubarb leaf. Tomato leaves can cause fever, rapid heart beat, delirium and convulsions; and rhubarb causes burning tongue and mouth. In all cases for first aid induce vomiting with syrup of ipecac which should be in all homes, along with activated charcoal to neutralize poisons, he said.
The third session dealt with high blood pressure and arteriosclerosis. Morse, son of a doctor who never taught him, said he was elated finally to learn how to take his own blood pressure. He said it was hard to hear on the stethoscope in the crowded Methodist parish house where the classes were held, but he finally got it.
One of the principles of the course is breaking through the mystique that surrounds physicians. Handling a stethoscope, even holding that scepter and symbol of medicine, and then pumping up a blood pressure cuff are part of that.
Dr. Taylor argues that taking one’s own blood pressure is not really self care unless one is hypertensive. “But it gives the patient new responsibility,” he said in an interview. “Taking blood pressure assumes that the responsibility is on you and you can learn to ask, ‘What is my body telling me?’”
He said the result of taking the course can change one’s style of living. “The content of the course is totally unimportant. I don’t know if everyone would agree with me on that, but basically blood pressure taking is not important in itself. What is important is that the action can make you a more active participant and dispel medical mystique.”
Other parts of the course included health insurance which wasn’t a great drawing card, according to Miss Irish. Dr. Taylor led discussion on listening and communicating which included helping the doctor and the nurse know when you do not understand and to ask questions.
One graduate said she got courage as a result of the course and dared to ask her gynecologist for her medical record. It turned out that he was willing.
Dr. Taylor said patients should learn to describe symptoms: location, type and frequency. Dr. Sehnert in his book suggests writing down questions on an index card which avoids forgetting everything in the examining room. “The Activated Patient (caps indicate a new breed) doesn’t leave the doctor’s office saying, ‘Gosh, what a doctor! He didn’t explain anything to me.’ The Activated Patient asks questions–lots of them,” writes Dr. Sehnert.
Dental care and skills involved the class in practice brushing and flossing with red dye tablets which show up the plaque.
Part seven of the course covered health and nutrition. Jackie Merrill, registered dietician at the hospital, described the American diet as having too many calories, too much fat and cholesterol, empty calories and lacking in bulk. She said that it was also missing whole grains, fresh fruits and vegetables and lowfat proteins.
Loretta Voyer, 36, of Peak’s Island, said that since the course she had cut down on Koolaid (the average American adult consumes 102 pounds of sugar a year, the nutritionist had said). She uses only one jug a week now and buys orange juice instead.
She also learned that she should be eating “one deep orange vegetable and one deep green vegetable every other day. She told us that frozen or canned produce is much better than old ‘fresh’ produce which isn’t fresh anymore.”
Mrs. Dinsmore, also from Peak’s, found that if given a choice a child will take an apple over a cookie. She now serves juice everyday as a result of the course. Mrs. Merrill helped participants examine diets to see strengths and weaknesses and suggested improvements.
Mrs. Burrill said she learned to keep the sugar bowl and the salt shaker off the table because they are already so high in American diets.
Mrs. Smith, a young mother of two on Chebeague, said she makes her children snacks of celery, carrots and peanuts in the shell to replace the cookies and pies she used to offer them.
Mrs. Swann, said she had been sure to have her glass of milk daily since the course ended in December.
Mrs. Merrill, the dietician, provided each student with a book list of 12 recommended books on nutrition and 50 not recommended. Among the no-no books–anything by Adele Davis or from the Rodale Press including Prevention magazine and Georges Ohsawa’s Zen Macrobiotics. “The AMA has said that Zen macrobiotics can be fatal especially to young children,” she said and recommended The Nuts Among the Berries by Ronald Deutsch.
“Common Illnesses and Injuries” occupied sessions 8 and 9, delineating what could be treated by oneself and when to call the doctor. A review covered the last session.
The Peak’s Island course, coordinated by Marcy Maguire, R.N., varied from the Chebeague curriculum. It included two sessions of CPR (cardiopulmonary resuscitation) and the Heimlich maneuver for emergency treatment of choking victims. They also had for the all-woman group breast self-examination and a sharing by a woman from Alanon, for spouses of alcoholics.
Mrs. Maguire said the Peak’s course takers used a different book from Dr. Sehnert’s and chose instead Take Care of Yourself; A Consumer’s Guide to Medical Care by Donald M. Vickery, M.D. and James F. Fries, M.D.
It has this to say about emergencies, for example: “Usually, the slowest way to reach a medical facility is by ambulance. It must go both ways and often is not twice as fast as a private car…”
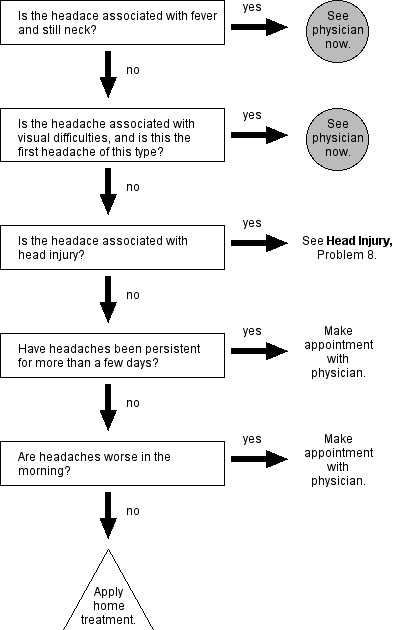
The book includes 68 flow charts enabling the consumer to decide when to treat himself and when to call the doctor. They range from hoarseness and nosebleeds to low back pain and headache.
This chart on headaches, “The most frequent single complaint of modern times tells when to apply home treatment and when to see the doctor.” From Take Care of Yourself.
Two people said after the course they were either thinking of changing their doctor or had changed. Mrs. Burrill said the course had given her the courage to consider changing. “I cannot talk to my doctor about the things that count. He is a young GP in a group, and I am sure he is competent, but I am dissatisfied. I have an annual physical which I feel better able to judge since the course, but I don’t get any feeling of response from him.”
She admitted that what she wanted was a confidant. She said her former doctor had listened through her highs and lows. She was sad to part with him when she moved to Maine. “I want someone who knows I am a healthy person and not a complainer,” she said.

William Swann said the most important point he got from the course was “Don’t panic if you don’t feel good or get a cut finger.”
Reta Morrill of Peak’s Island said that after the course her son cut his knee and “there was a whole lot of blood” but she remained calm and confident when she went to pick him up at the school yard. She took him to the health center where the nurse practitioner used Steri-strips to close the wound which did not require sutures.
She said she also learned to treat burns with cold water, not butter or grease, and when her two-year-old burned himself she covered the burn with ice cubes. When her son got poison ivy, Marjorie Erico, the nurse, told her to wash him with baking soda. For sunburn she recommended a vinegar solution.
Carolyn Swann said one thing she got from the course was giving Dr. Sehnert’s book to her daughter in New Hampshire. The daughter used the book to diagnose her strep throat which convinced the doctor finally to take her throat culture, which he had been resisting. It turned out that both she and her husband had been infected with strep. “The book paid for itself in that incident alone,” she said.
About half of one per cent of the $140 billion spent on health last year went to health education. As Dr. Taylor pointed out: “I am sure you know the comparisons of $24 million spent on health education in this country compared with $27 million for Alka Seltzer commercials alone.”
Dr. Sehnert said a current ad campaign for Real cigarettes is costing $500 million and includes the biggest sign in Times Square, one and a half trainloads of billboard posters and 2,000 new salesmen.
By comparison he said there were only three persons working in health promotion in HEW in Washington and 20 working at the bureau of health education in Atlanta for the whole country.
The charge for the Maine islands programs was $1 per session per person. The full cost was about $1,500.
Dr. Taylor said plans are in the works for more courses at Peak’s and Chebeague. The husbands of the Peak’s women want a CPR course, and Ned Morse expects it won’t be hard to get 24 more persons to sign up after Labor Day. Dr. Taylor envisions a course for hospital personnel and high school faculty or seniors, it’s not clear yet which.
Also there is a nearby town of Kezar Falls which is medically underserved where he would like to see a course.
Miss Irish, who coordinated the Chebeague course, said, “It is hard to determine whether there was a change in behavior because of the course. You can’t measure things like that definitely.”
That’s a problem with patient education; it is hard to prove to the government or to a foundation that you are getting results. But it seems to me that if more patients have health knowledge and don’t feel like dummies in front of the doctor and aren’t afraid to ask questions the health world is going to be happier.
Received in New York on July 22, 1977
©1977 Phil Weld, Jr.
Phil Weld, Jr. is an Alicia Patterson Foundation award winner on leave from the Lawrence Eagle-Tribune. His fellowship subject is the role of self-care in health: a look at prevention, patient education and patient power in the U.S. and Canada. This article may be published with credit to Mr. Weld as a Fellow of the Alicia Patterson Foundation and to the Lawrence Eagle-Tribune. The views expressed by the author in this newsletter are not necessarily the views of the Foundation.








